It has now been ten years since the general use of gel filled breast implants has ended. Except for unusual circumstances, patients in the US all receive saline filled implants. Although admittedly, there is a higher incidence of rippling, or surface irregularity, with these implants, the added safety more than offsets this disadvantage.
Gel implants were widely used for over 25 years and enjoyed a high degree of safety. As reported in the January 2002 edition of Plastic Surgery Products, there are more than 20 epidemiological studies that have failed to show any relationship between the use of breast implants and connective tissue disease. Nonetheless, these studies have not addressed the incidence of local complications following rupture of these devices.
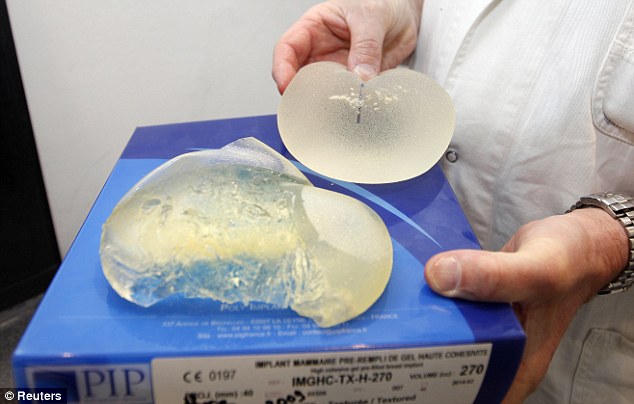 OLDER IMPLANTS MORE LIKELY TO LEAK
OLDER IMPLANTS MORE LIKELY TO LEAK
There is no avoiding the acceptance that many of the older gel filled implants have lost their integrity over the years resulting in leakage of silicone gel. In many cases, the gel is contained by the fibrous capsule, or scar tissue, that surrounds the implant. If the surrounding scar tissue does not contain the gel, migration into surrounding tissue occurs which can lead to local inflammatory disease, lymph node enlargement and possible nerve injury. Often this leakage results from the old practice of treating firm breasts with “external capsulotomy,” in which the surgeon would squeeze the breast with enough force to break open the scar tissue. Unrecognized at the time was the fact that often the implant was broken as well as the scar tissue.
In the late 1980s, most companies manufacturing breast implants began using a thicker silicone membrane around the implant, which greatly reduced the incidence of shell rupture.
FDA STUDIED EFFECTS OF GEL LEAKAGE
Last year, the FDA published the results of a study on the effects of gel leakage from silicone gel filled implants in the Journal of Rheumatology. The study was prompted by concerns that leakage might lead to problems unknown or unsuspected. They were also concerned since implant rupture represented a failure of the device, which was no longer performing as it was intended.
The study indicated that women who had implant rupture, based on magnetic resonance imaging (MRI), without spread of gel through the capsule were no more likely to report symptoms or diagnosis of autoimmune type diseases or disorders. Women with rupture, and MRI evidence of gel leakage, were 2.8 times more likely to report symptoms of diagnosis of fibromyalgia, but no more likely to report any of the other autoimmune diseases.
WHAT IS FIBROMYALIGIA?
Fibromyalgia is a non-specific syndrome which includes complaints of soreness and weakness with associated symptoms of fatigue, poor sleep, anxiety and irritable bowel symptoms. The stiffness and pain is frequently gradual, diffuse and achy and is generally aggravated by straining or overuse. Laboratory studies for other specific rheumatoid disorders are typically normal. There is no specific treatment for fibromyalgia. It often remits when there is decreased stress. Treatment is largely directed at relieving the symptoms with pain medication, exercise, massage, and often with antidepressants.
Because of the non specific nature of the disorder, if is impossible to know whether the gel leakage is responsible for the problem, or if it simply relates to patient anxiety over other possible problems related to the implants.
There is also no evidence to indicate whether removal of the implants and replacement with saline filled implants would improve the condition, although other studies have suggested this.
The data does seem to confirm the advisability of women with ruptured gel implants to seriously consider having them replaced with saline filled devices. While the FDA depended on MRI for diagnosis of rupture, our experience has convinced us that endoscopy is the surest way to diagnose rupture. Endoscopy allows direct inspection of the implant and the surrounding capsule. If the implant is intact, there need be little concern over the possibility of gel migrating into surrounding tissue.
WHAT DOES IT ALL MEAN
It remains our belief that currently, saline filled implants represent a safer alternative, compared to the older gel filled devices. While newer implant technology may lead to safer devices, our current recommendation is that saline filled implants represent the wiser choice for patients considering breast augmentation today.


